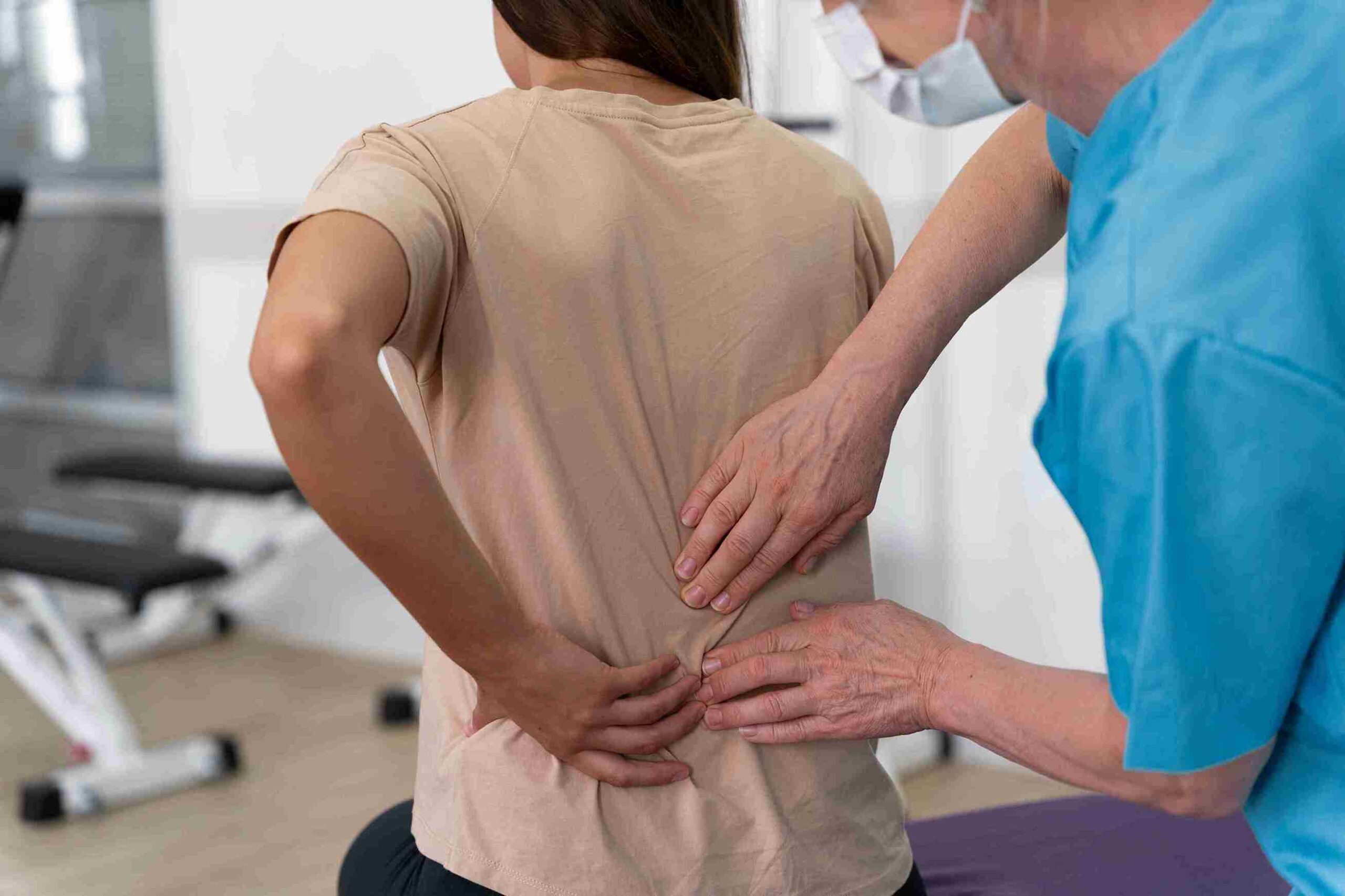
Quick Summary: What Is Lower Back Pain and How Can I Cure It?
- Most common cause: Muscle strains and sprains are the primary source of lower back pain.
- Red flags that need immediate medical attention: Loss of bladder or bowel control, severe leg weakness, numbness in groin area, or pain with fever.
- Safe stretching: Gentle stretching helps chronic pain. As much as possible, avoid aggressive stretching during acute flare-ups.
- Treatment plan: Start with conservative methods (movement, stretching, physiotherapy) before considering injections or surgery.
What is Lower Back Pain?
Lower back pain affects nearly everyone’s life at some point. The scale is staggering. Around 619 million people suffered from it worldwide in 2020, and experts predict this will rise to 843 million cases by 2050.
Your lumbar spine carries the weight of your upper body while allowing you to bend, twist, and move in countless directions each day. The combination of heavy load and frequent movement makes this area particularly vulnerable to stress and injury.
Your lower back consists of five vertebrae, muscles, ligaments, and intervertebral discs that work together as a complex system. When any part of this system becomes irritated, strained, or damaged, you feel pain. The area experiences constant stress from daily activities like sitting, standing, lifting, and even sleeping in awkward positions.
Types of Lower Back Pain
Lower back pain falls into three main categories based on how long symptoms persist.
Acute Pain
Acute pain appears suddenly and lasts less than six weeks. It’s the most common type and usually resolves on its own with proper care. You might experience acute pain after:
- Lifting something heavy with poor technique
- Making a sudden twisting movement
- Sleeping in an awkward position
- A minor fall or impact
The pain typically stays localised in your lower back and responds well to rest or gentle movement.
Subacute Pain
When pain persists between six to twelve weeks, it enters the subacute phase. Subacute pain often indicates that your initial (acute) injury hasn’t fully healed or that contributing factors like poor posture or weak muscles are preventing recovery. This is the ideal time to seek physiotherapy to solve the pain before they become long-term problems.
Chronic Pain
Pain lasting more than twelve weeks is considered chronic, which can be continuous or come and go in episodes. It’s normal for this pain to get progressively worse over time. Chronic lower back pain frequently involves multiple factors including:
- Muscle imbalances
- Joint problems
- Disc degeneration
- Nerve involvement
Unlike acute pain, chronic lower back pain requires a comprehensive treatment that covers strength deficits and lifestyle factors that contribute to ongoing pain.
What Causes Lower Back Pain?
Knowing what triggers your lower back pain helps you choose the right treatment and avoid future problems.
Mechanical Issues
This is by far the most common type, accounting for the majority of cases we see in Rehab Lab Physio. Mechanical pain comes from problems with your spine’s moving parts, including the muscles, joints, ligaments, and discs. You’ll typically feel:
- Aching or stiffness that worsens with certain movements
- Pain that improves with rest or position changes
- Muscle spasms or tightness
- Localised discomfort in your lower back
Nerve-Related Pain
You experience a distinctly different type of pain when spinal nerves become irritated or compressed. For this case, the pain is sharp and shooting. It also often travels beyond your lower back into your buttocks and legs.
The most recognisable form is sciatica, where pain follows the path of your sciatic nerve down your leg. You might also experience numbness and tingling in the affected areas.
Pain from Other Medical Conditions
Sometimes, pain in that area signals an underlying medical condition rather than a simple mechanical problem. Inflammatory conditions like ankylosing spondylitis cause persistent stiffness and pain that improves with movement but not rest. Infections, tumours, or kidney problems can also manifest as back pain.
Degenerative Causes
Disc degeneration occurs naturally as you age. Your spinal discs lose water content and become less flexible, making them more prone to tears or herniation. Moreover, facet joint arthritis develops when the cartilage covering your spinal joints wears away, creating bone-on-bone contact and inflammation that are particularly noticeable in the morning.
Back Pain From Running
Running creates repetitive impact forces that travel up through your legs into your spine. Poor running technique, particularly overstriding or heel striking, increases these forces significantly, which causes lower back pain.
Training errors contribute to many running-related back injuries. Increasing your distance or intensity too quickly doesn’t allow your body time to adapt. Your core muscles, which support your spine during running, may not be strong enough to handle the increased workload.
Additionally, running on uneven surfaces creates imbalances that stress your lower back. Wearing worn-out running shoes that already lost their shock-absorbing properties also transfers more impact to your spine.
Lifestyle Factors
Hunching over computers, craning your neck forward to read screens, and remaining stationary for hours creates the perfect storm for lower back problems. Many office workers develop what we call “desk posture,” involving rounded shoulders and a forward head position. Getting a standing desk is recommended if you want to avoid this issue.
Nerve involvement creates distinctive symptoms. Sharp, electric-like pain that follows a specific path down your leg suggests nerve compression. This often comes with changes in sensation or muscle strength in the affected leg.
How Can I Reduce My Lower Back Pain?
Understandably, you want fast relief when lower back pain hits you. The good news is that most episodes respond well to simple, science-based treatments.
Immediate Relief Methods
Gentle movement works better than complete rest if you’re dealing with acute pain. Walking, even for just five minutes every hour, maintains blood flow and prevents stiffness from developing. Apply ice for 15-20 minutes during the first 48 hours to reduce inflammation. After this initial period, heat therapy helps relax tight muscles and improve circulation.
Anti-inflammatory medications like ibuprofen can provide short-term relief. However, use them as directed and don’t rely on them as your only treatment strategy.
Seek Professional Treatment
Physiotherapy solves both your symptoms and underlying lower back pain causes (if there’s any). Professionals can assess your movement patterns to identify muscle imbalances, and create targeted exercise programs to restore function and prevent recurrence.
Manual therapy techniques like dry needling and cupping can provide immediate relief while improving your spine’s mobility.
Frequently Asked Questions
What not to do with lower back pain?
Extended bed rest weakens your muscles and often prolongs recovery. Your body needs movement to heal properly, so aim to stay as active as your pain allows. Pushing through severe pain during exercise can worsen your injury so respect your body’s signals and modify activities rather than stopping completely.
How to create your personal prevention plan?
Assess your daily activities and identify positions or movements that trigger your lower back pain. Modify your workstation, sleep setup, and exercise routine to address these factors. It’s always better to seek the help of professionals for long-term treatment.
How can I reduce my lower back pain immediately?
Start with gentle movement, apply ice for acute pain or heat for chronic pain, take anti-inflammatory medication as needed, and consider physiotherapy for persistent symptoms.
Is it okay to stretch lower back pain?
Yes, gentle stretching helps chronic lower back pain, but avoid aggressive stretching during acute flare-ups as it may worsen symptoms.
How do I tell if my lower back pain is serious?
Seek immediate help for loss of bladder/bowel control, progressive leg weakness, severe pain with fever, or pain that keeps you awake at night.
How do you tell if lower back pain is muscle or disc?
Muscle pain feels like a dull ache that improves with rest, while disc pain is sharp, may shoot down your leg, and often worsens with sitting.
How can I release lower back pain?
Gentle self-massage using a tennis ball or foam roller can help release muscle tension. Paced breathing exercises can also activate your parasympathetic nervous system, helping reduce pain perception. Finally, change positions frequently throughout the day.
Most lower back pain resolves with appropriate self-care and gradual return to activity. However, persistent or worsening symptoms warrant professional assessment to develop a proper treatment plan. Remember, early intervention often leads to better outcomes and faster recovery. Our experienced physiotherapists at Rehab Lab Physio can help you take the first step towards having a pain-free lower back. Reach out to us today for a complete assessment.